Mainly acute allergic and seasonal conjunctivitis associated with rhinitis in 50-90% of cases, they result from a hypersensitivity to a conjunctival allergen environment.
The evocative events:
1) Itching especially of the eyelids and inner corners
2) The conjunctival redness
3) The presence of a watery
4) The swelling of the eyelids
5) history of eczema of eyelids
6) The sensation of a foreign body
7) Photophobia
8) The existence of impaired fixation, convergence, eye syndrome irritable at the computer.
We must remember that allergic eye is red, swollen, itchy and wet.
Allergic conjunctivitis in a child of 13 years.
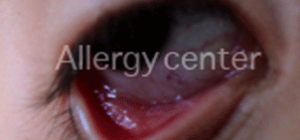
Allergy testing:
Skin tests: skin prick tests to common allergens often possible to find the offending allergen.
The laboratory diagnosis of allergy
Blood eosinophilia
Serum IgE
Testing of multi-allergen screening
Assays of IgE in tears.
Research of eosinophils in tears normally present in tears and the superficial layers of the epithelium, their presence towards a manifestation of allergic.
The conjunctival challenge test: to carry out after cessation of any allergy treatment. It consists to involve contacting the allergen with the conjunctiva. Immediate reaction with redness, tearing may appear in the half-hour.

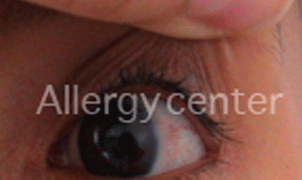
Conjunctival challenge test positive for mites
In a child of 12 years, with negativeallergy tests, despite a very suggestive clinical symptoms of allergy.
There are different forms of allergic conjunctivitis:
A. THE ACUTE SEASONAL CONJUNCTIVITIS
They are often associated with seasonal rhinitis.
Often affect the two eyes
The beginning is usually sudden after allergen exposure by an ocular itching, tearing, conjunctival redness and swelling of the eyelids reducing the palpebral fissure.
Diagnosis will be guided by clinical and confirmed by skin tests
Ocular provocation tests are rarely needed.
The differential diagnosis may arise, however, with:
Traumatic acute conjunctivitis
Infectious conjunctivitis (viral + +)
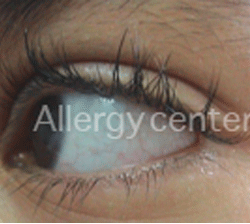
Acute seasonal conjunctiva in a 11 years old child. Positive skin prick tests to grass pollen.
TREATMENT:
Allergen avoidance
Antihistamine eye drops or oral
Degranulating eye drops
Short course of corticosteroids never more than 15 days and with the approval of the ophthalmologist
TUNISIAN CENTER FOR EXPLORATION OF ALLERGIC DISEASES
B. THE CHRONIC CONJUNCTIVITIS
Manifested by ocular pruritus located under the eyelids in the inner corner, with swelling, conjunctival redness, chronic tearing, tingling sensation of sand in the eye. These signs dominate the night and in the morning upon waking.
These bilateral signs are usually associated with rhinitis.
Examination reveals a papillary conjunctivitis with eyelid redness and papillary formation.
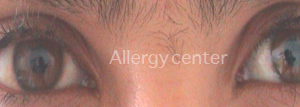
The use several drops can lead to iatrogenic disease such as glaucoma.
The diagnosis is clinical oriented reinforced by the practice of allergy tests.
Sometimes, we need to perform an ocular challenge test to know the allergen if the prick test are negative, or if the patient has polyallergy to identify the allergen responsible.


Annual per chronic conjunctivitis by allergy to dust mites.
Inflammation and follicles visible on reversal of the eyelids.
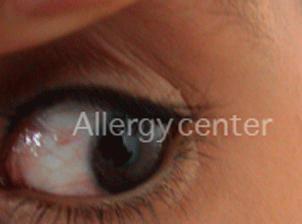
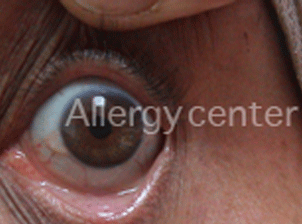
TREATMENT :
a) Ovoiding of the offending allergen
b) Not given corticosteroids
c) Degranulating mast
d) Anti-histamin therapy
e) Desensitization
C. THE VERNAL KERATO-CONJUNCTIVITIS
Eye disease easy to diagnose but poses therapeutic problems.
Clinical signs:
It primarily affects boys and essentially begins between 2 and 10 years. It is bilateral and asymmetrical willingly. It is mainly triggered by sunlight explaining it may exceed on spring an summar. In hot countries it is perannual.
The signs are intense with some impact on school life of the child as it causes itching, intense pain, redness, tearing and photophobia uncontrollable (fear of light).
On examination we note the presence of whitish filaments or false membranes in the conjunctiva. The child refuses to light.
These lesions are seated electively at the upper eyelid and conjunctiva in limbo. The turning of the eyelid find the traces of the upper palpebral conjunctiva .
All these aspects are aggravated by heat, sun, allergic conditions and long term use of corticosteroids.
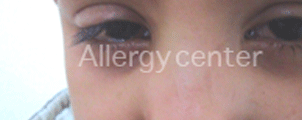
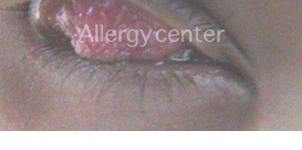
Vernal conjunctivitis, giant papillary with a child of 8 years.
Paraclinical:
Conjunctival smear or biopsy: infiltration by eosinophils
IgE levels in tears
The allergy testing are positiv in 50% of cases.
Evolution and prognosis: some complications may occur :
a) superficial punctate keratitis
b) Corneal ulcer. The ulcer may be the site of neovascularization and severe loss of visual acuity.
Moreover, the evolution is toward spontaneous resolution within 2 to 10 years in a totally unpredictable manner. Sometimes optical effects (astigmatism) can apprear. Evolution can be towards atopic keratoconjunctivitis
TREATMENT:
Allergen avoidance in atopic subjects
General measures: sunglasses + + repeated washing of the eyes with saline
Application of cold compresses
Fight against the tendency to rub eyes
Antidégranulant
Topical corticosteroids: results in improved but risk of severe glaucoma, cataracts and lower resistance to infection so use short courses.
Cyclosporine eyedrops 2% may be beneficial
Acetylcysteine eye drops or systemically for the filaments
The desensitization in allergic subjects
If surgical treatment of corneal ulcer, or the presence of vernal plate (scraping or peeling)
Cryotherapy
D. THE ALLERGIC KERATO-CONJUNCTIVITIS
It appears in adulthood around 30-40 years and most often affects the male subject. It is often associated with atopic eczema
Clinical picture:
Functional signs are often major with intense itching, eye burning sensation, photophobia, tearing, sweating and eczema of the eyelids.
This table grows with a constitutional eczema.
Many complications can appear
Conjunctivitis, atopic keratoconjunctivitis in a man of 30 years.
A herpes or staph superinfection
Dry eye is an inevitable consequence of conjunctivitis
Astigmatism and cataracts.
Additional tests:
The association with atopy and eczema oriented diagnosis
Usual allergy tests should be performed
TREATMENT:
Routine anti-allergic measures
Topical steroids over a short period
If severe form corticosteroids
E. CONJUNCTIVITIS GIGANTOPAPILLARY
This is not an allergic disease. It concerns patients with contact lenses . The eyelid damage is evident when returns the upper eyelid with the identification of giant papillary 1 mm invading part of the surface of the eyelids.
The clinical symptoms are suggestive but histological studies show infiltration by eosinophils and basophils. Similarly, we may have a hyper-IgE
TREATMENT:
Remove the officer, careful cleaning, degranulating mast.